By Daniel Fontaine

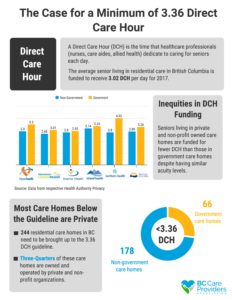
The initial release of the Office of the Seniors Advocate’s (OSA) Quick Facts Directory in 2016, along with the subsequent media attention, highlighted a number of challenges facing residential care homes in British Columbia – particularly the need for increased staffing levels for seniors in residential care.[i] The Quick Facts Directory outlined that of the 292 government-funded care homes in B.C., 232 did not meet the ministry’s staffing guideline, a recommendation of 3.36 hours of care per senior every day.[ii]
As a result of the OSA report, the BC Ministry of Health announced in early April 2016 that it would be undertaking a review of staffing guidelines in government-funded long-term care homes for seniors. In particular, BC Heath Minister Terry Lake requested the Ministry undertake a review to examine how health authorities are funding seniors’ homes, including looking at the care hours being provided to seniors, especially those living with dementia and other ailments.[iii]
Though originally intending to release their review of Direct Care Hours in the early fall of 2016, the Ministry of Health report, and any accompanying investments, are still forthcoming. The intervening months, however, have not made this issue any less urgent; this January, the OSA published a 2017 update of the Quick Facts Directory, which highlighted the fact that 90% of B.C.’s care homes are still not meeting the 3.36 hours of staffing care per day recommended in the provincial government guidelines. [iv] The average non-government care home in BC is funded for just 2.89 Direct Care Hours per resident each day, well below the 3.36 guideline (see infographic).
In order to provide further insight into the challenges that exist regarding staffing levels in BC’s residential care homes, the BC Care Providers Association (BCCPA) would like to place this complex issue into the proper context, thus highlighting why further investments in this area are needed.
Staffing levels, more formally referred to as Direct Care Hours (DCH), reflect the time that healthcare professionals, including Registered Nurses, Licensed Practical Nurses, Physio and Occupational Therapists, Residential Care Aides and others, dedicate to caring for their residents each day. While still important for seniors quality of life, DCH do not include non-medical hospitality services such as meals, laundry or housekeeping.
In BC, like most provinces, there are no specific provincial requirements for a number of DCH that must be provided on average to each resident per day. Likewise, there are no specific requirements for the type or mix of staff that must be on duty. Instead, there are, however, some outcome-based staffing standards, which are contained in the Community Care and Assisted Living Act (CCALA) and accompanying residential care regulations.[v]
However, in 2009, the BC Ministry of Health did provide the regional health authorities with a framework to assist in the development of their three-year plans. The health authorities used cost assumptions provided by the framework to ensure plans reflected a consistent provincial approach to residential care staffing. In particular, one of the cost assumptions was that there would be 3.36 hours of direct care provided per day per resident (3.00 hours nursing and 0.36 allied, or supporting care).[vi] The Ministry, however, has indicated clearly that this number of DCH was to serve only as a guide for health authorities.[vii]
The Ombudsperson’s 2012 report on seniors care also recommends that the BC Ministry of Health establish appropriate staffing mixes including a minimum number of DCH and number of staff required at different times in residential care homes. Likewise, the report recommended the Ministry work with health authorities to conduct an evaluation to determine whether residential care budget in each health authority is sufficient to meet the current needs of its population; and establish consistent method to determine funding requirements of residential care homes.[viii] The same report also notes that the costs of moving to the 3.36 can be quite significant.
Despite these fiscal challenges, 3.36 DCH may be a bare minimum. A study from the Canadian Centre for Policy Alternatives, entitled Promising Practices in Long-Term Care, concludes that “direct care staffing should be set at a minimum of 4.1 hours per resident each day.”[ix] A survey of over 750 British Columbians conducted by the BCCPA identified that the top priority for any new investments in seniors’ care were increasing staffing levels in care homes, followed closely by increasing access to home care.[x]
Apart from increasing the overall level of funding for staffing levels, British Columbians have also identified greater equality in staffing as a priority. According to a 2015 Insights West survey of over 800 British Columbians commissioned by the BCCPA, 78% of respondents believe regardless of where you live, the number of DCH funded by Health Authorities for a senior with similar levels of acuity should be the same.
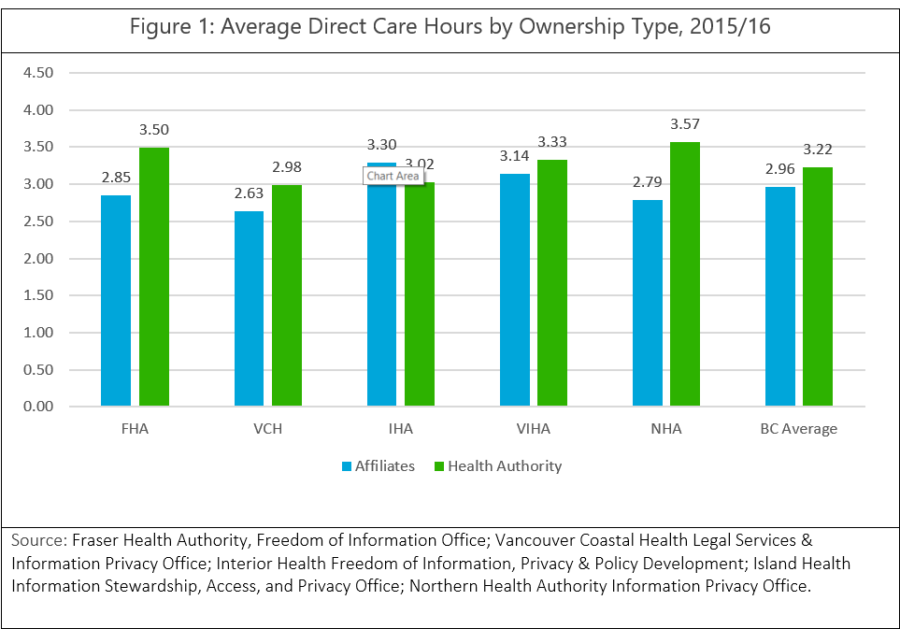
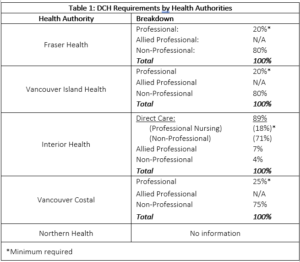
And yet, the BCCPA’s own investigation into DCH has found that significant disparities exist both between and within the Health Authority regions. These variations are particularly stark when care homes are broken down by ownership type. As demonstrated in Figure 1, in each health authority region, the non-government care providers are funded for fewer DCH on average than government owned and operated care homes.[xi] This is further exacerbated by the fact the skill mix of staff included in a ‘direct care hour’ differs from health authority to health authority (see Table 1). With such disparities, it makes it difficult to provide equal and consistent levels of care, leaving some seniors at a disadvantage over others.
It is for these reasons that the BCCPA’s Strengthening Seniors Care report recommends that the Ministry of Health invest $230 million per year to move to a minimum of 3.36 DCH per resident per day at each residential care home.[xii] The report further recommends that, in order to increase transparency and accountability, that a standard definition of DCH be developed by the Ministry of Health and the Health Authorities in partnership with the sector by 2017.
 Likewise, as recommended in 2015 BCCPA report entitled Quality, Innovation, Collaboration: Strengthening Seniors Care Delivery in BC it advocates that Health Authorities redirect a minimum of 1% annually over a five-year period to the home and community care sector. The BCCPA believes not only could this help deal with existing cost pressures facing service providers it could help support development of new care models, particularly new Continuing Care Hubs in order to better meet current and future DCH requirements.[xiii]
Likewise, as recommended in 2015 BCCPA report entitled Quality, Innovation, Collaboration: Strengthening Seniors Care Delivery in BC it advocates that Health Authorities redirect a minimum of 1% annually over a five-year period to the home and community care sector. The BCCPA believes not only could this help deal with existing cost pressures facing service providers it could help support development of new care models, particularly new Continuing Care Hubs in order to better meet current and future DCH requirements.[xiii]
The BC Care Providers Association (BCCPA), which in general supports the DCH review, looks forward to discussing the care hours being provided to seniors with the Ministry of Health, as well as on the development of any new strategies to deal with health human resources issues more generally. The BCCPA believes that further government reviews on DCH and funding should address the importance of seniors in residential care homes in receiving sufficient staffing levels. The BCCPA will continue advocating to ensure that non-government care operators can remain financially viable while providing seniors with high quality care.
View Fontaine’s original Op-Ed: Direct Care Hours
END NOTES
[i] BC Office of the Seniors Advocate. Residential Care Facilities: Quick Facts Directory. January 2017. https://www.seniorsadvocatebc.ca/app/uploads/sites/4/2017/01/Residential-Care-Quick-Facts-Directory-2017.pdf .
[ii] Vancouver Sun. Most senior nursing homes miss Ministry of Health staffing guideline. April 6, 2016. http://vancouversun.com/news/local-news/vast-majority-of-senior-nursing-homes-below-the-ministry-of-healths-staffing-guideline
[iii] Vancouver Sun. BC Health Minister Orders Review of Staffing Guidelines in Long-Term Care Homes for Seniors. April 7, 2016. http://vancouversun.com/news/local-news/b-c-health-minister-orders-review-of-staffing-guidelines-in-long-term-care-homes-for-seniors
[iv] The Ashcroft Cache Creek Journal. Updated guide to residential care facilities in BC shows care has grown worse in some areas. February 7, 2017. http://www.ash-cache-journal.com/news/413086303.html
[v] As outlined in Section 42 (1) of the Residential Care Regulations: A licensee must ensure that, at all times, the employees on duty are sufficient in numbers, training and experience, and organized in an appropriate staffing pattern, to (a) meet the needs of the persons in care, and (b) assist persons in care with activities of daily living, including eating, mobility, dressing, grooming, bathing and personal hygiene, in a manner consistent with the health, safety and dignity of persons in care. To access Residential Care Regulations, click here: http://www.bclaws.ca/Recon/document/ID/freeside/96_2009
[vi] Home and Community Care Program, “Costing Assumptions #3 for the Proposed Staffing Framework for Residential Care Facilities,” 11 August 2009, 1.
[vii] Home and Community Care Program, “Residential Care Staffing and Reporting Tool Frequently Asked Questions,” internal document, 3.
[viii] Ombudsperson. The Best of Care: Getting It Right for Seniors in British Columbia. Part 2. February 2012. Accessed at https://bcombudsperson.ca/documents/best-care-getting-it-right-seniors-british-columbia-part-2 . In research and consultations conducted by the Ombudsperson they found that the recommended range of care hours was generally between 3.2 and 4.0 hours per resident per day.
[ix] CUPE back Gélinas bill to mandate at least 4 hours of care per long-term care resident. Nov 24, 2016. https://www.sudbury.com/local-news/cupe-back-gelinas-bill-to-mandate-at-least-4-hours-of-care-per-long-term-care-resident-472741
[x] Final Report BCCPA Public Consultation Survey. October 2016. https://bccare.ca/wp-content/uploads/2016/10/Public-Consultation-Survey-Report-Final-October-2016.pdf
[xi] The BCCPA obtained this data by filing individual freedom of information requests to each regional health authority in BC.
[xii] BCCPA. Strengthening Seniors Care: A Made in BC Roadmap. January 2017. https://bccare.ca/wp-content/uploads/2017/01/BCCPA_Roadmap_ExecSummary_Jan2017.pdf
[xiii] BCCPA. Quality-Innovation-Collaboration: Strengthening Seniors Care Delivery in BC. September 2015. Accessed at: https://bccare.ca/wp-content/uploads/BCCPA-White-Paper-QuIC-FINAL-2015.pdf.